Our first project in Chad powers fistula surgeries
In Chad, obstetric fistula affects thousands of women, yet many don't know it can be treated. For those who do, the vast distances, few specialists, and little infrastructure mean women often live with the painful condition for years before accessing surgery. Village des Femmes in Abéché is one of only two clinics alongside N'Djaména's treatment centre that can, but until recently, it was running on an expensive and unreliable diesel generator. In collaboration with Women's Hope International, we replaced it with solar, opening the door to almost 1200 additional treatments over the next decade.
A 27 kWp PV system, spanning two roofs now powers the majority of the buildings at Village des Femmes, Abéché
A Region in Crisis
The Ouaddaï Province of eastern Chad sits at the crossroads of one of the world's most severe humanitarian emergencies. Since 2023, the civil war in neighbouring Sudan has driven more than 1.2 million people across the border into Chad.
In 2025 alone, over 179,000 new arrivals reached the region, 87% of them women and children. This influx has placed already-strained health services under enormous pressure.
Chad has one of the world's highest maternal mortality rates, at approximately 1063 deaths per 100,000 live births (2023), roughly 260 times higher than Germany's rate of 4.1 (2022).Alongside these death tolls sits obstetric fistula. A devastating birth injury that, for many survivors, means a lifetime of suffering.
Understanding obstetric fistula
When labour is severely obstructed and no skilled health personnel is available, the ordeal can continue for days. The prolonged pressure of the trapped baby against the mother's tissues cuts off blood flow. When that tissue dies and falls away, a hole, a fistula, is left in the birth canal, either between the bladder and vagina, or between the rectum and vagina.
The consequences are devastating from constant incontinence, recurring infection, and profound social isolation. Research suggests that around 90% of women who develop obstetric fistula end up delivering a stillborn baby. Women who survive are frequently abandoned by their communities.In high-income countries, access to timely caesarean sections has nearly eliminated fistula. In Chad, however, where most women give birth far from any medical facility, it remains a largely hidden epidemic. Available research suggests an incidence rate of around 2.1%, which could translate to roughly 500-1,000 new cases each year. Yet only a small number of specialist centres provide surgical repair, collectively performing an estimated 250-300 surgeries annually, leaving many women waiting years for care.
Housna Youssouf Mahamat, Senior Midwife at Village des Femmes, seen during a patient consultation. © Kevin Doumdedje / Women’s Hope
A Specialist Clinic with a fragile foundation
Located in Abéché, the provincial capital of Ouaddaï, the Village des Femmes ("Women's Village") sits within the premises of the University Hospital of Abéché and is one of the few centres in Chad dedicated to treating obstetric fistula survivors. Led by Professor Dr. Valentin Vadandi, it is recognised as a top-level centre that handles the country's most complex cases and occasionally patients from neighbouring countries. Its status within the hospital is somewhat ambiguous, neither fully autonomous nor strongly supported by the institution, a reflection of how little priority obstetric fistula receives in the broader healthcare system. Despite operating with scarce resources, it performs around 100-150 surgical repairs each year, providing not only surgical care but also the medical and psychological aftercare women need to rebuild their lives.
Women's Hope International (Women’s Hope) has been operating and supporting health facilities in eastern Chad since 2015, with a focus on strengthening the local healthcare care system through infrastructure expansion, training of health professionals, a strong component of community involvement, even in such a difficult area as improving patient transport. The Women's Village is a central part of their mission in the region.
But for all of Women's Hope dedication, the facility faced a fundamental problem: electricity. Only around 12% of Chadians have access to national electricity and in rural areas, that figure drops to near zero. The Women's Village had been running on a small diesel generator with an operating theatre that cannot afford interruptions. Lighting, surgical equipment, monitoring devices: none of which can stop mid-procedure. With volatile fuel prices and supply lines increasingly strained by shortages and the ongoing Sudan crisis, the generator was a fragile foundation.
It was this challenge that brought Aid Pioneers and Women’s Hope together.
How it came together
Chad lies in the tropical sunbelt of Africa, with some of the highest solar irradiance on the continent. The conditions for solar power are exceptional, but the challenge is actually doing it.
That is exactly what Aid Pioneers is built for. Through our in-house solar engineering team we handle the full journey: from designing a system around actual energy demand, to managing international shipping and logistics, to supporting the local installation team on the ground, and maintaining remote monitoring once the system is live.
Through our partnership with Enpal, we are able to procure and deliver high-quality equipment that would otherwise be largely unavailable in Chad. Solar equipment is hard to come by here for reasons that go beyond budget. The market is underdeveloped, purchasing power for quality equipment is limited, and the logistical reality of a landlocked country with little transport infrastructure outside the cities makes supply chains deeply unreliable.
For this project, getting the equipment to site meant coordinating a route from our warehouse in Chemnitz to Hamburg, by sea to Cameroon, by cargo train to N'Djamena, and a final truck leg to Abéché. It is rarely straightforward, and this project was no exception. But that is the work and it is exactly the kind of complexity that stops many organisations from trying in the first place.
None of that would have been possible without Women’s HopeI's decade of on-the-ground presence in eastern Chad. Community trust, local coordination, and knowledge of how the facility actually operates.
For the Women's Village, we designed the system specifically around the facility's real consumption profile, with particular attention to the needs of the operating theatre. We selected FoxESS equipment, chosen not only for its performance and long warranty, including a feature that proves critical in practice: smart shutdown protection.
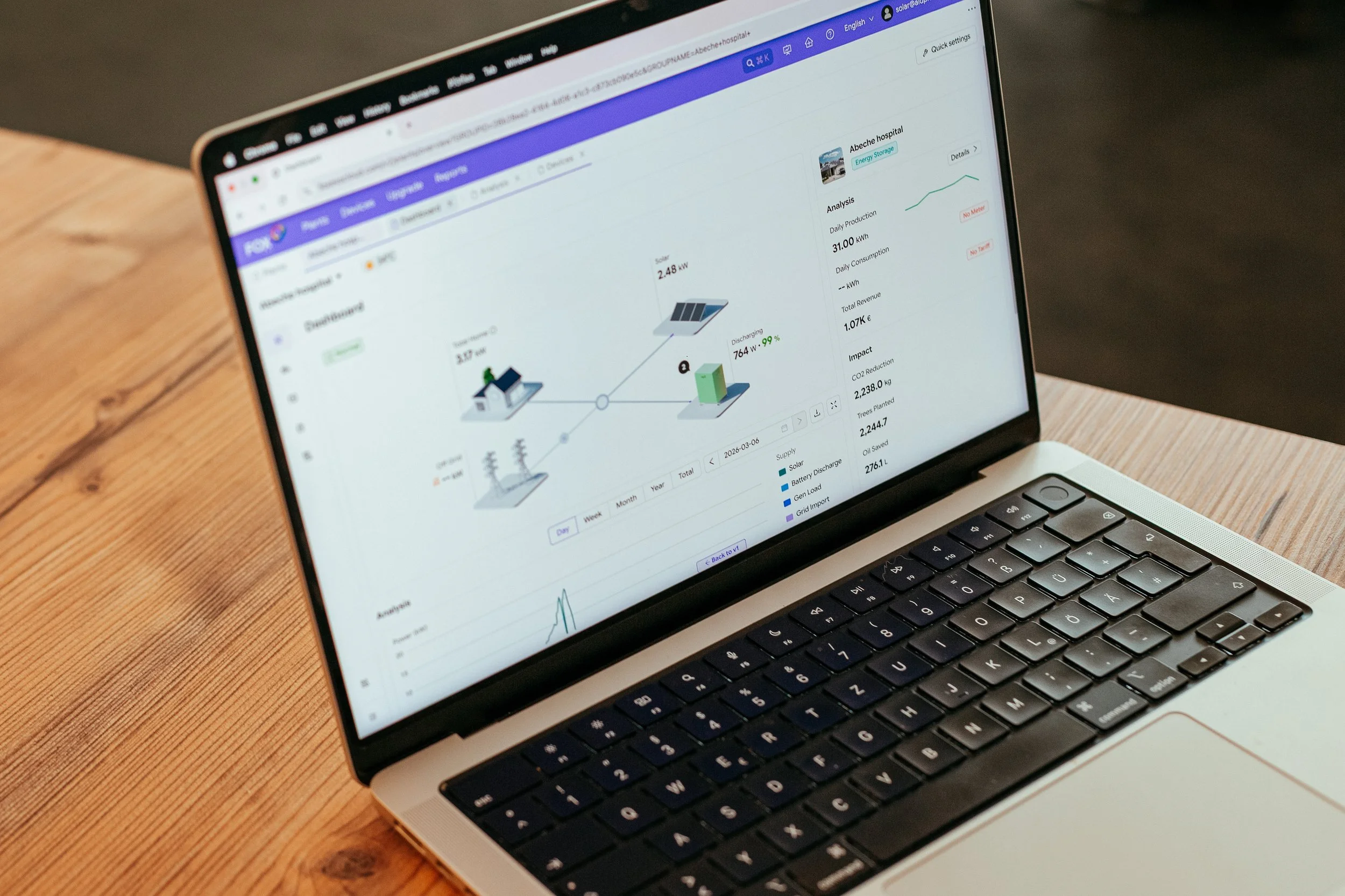
FoxESS remote monitoring platform for the Abéché installation, providing shared access for all project partners to monitor system performance.
When the system failed and how we knew
Since installation, the system has experienced two faults. The first was caused by the clinic overloading the system by connecting more devices than it was configured to handle. The second was a grid fault. In both cases, our engineering team in Berlin was able to read the error codes, diagnose the fault remotely, and walk the team in Abéché through the resolution process, minimising the need for local technical intervention on site.
That last point is important. In places where solar infrastructure is still being built out, the nearest qualified technician is often based in the city, which leaves remote facilities waiting for days until someone can make the trip. Remote monitoring removes that dependency in most cases and keeps the cost of maintenance where it should be and as low as possible.
This is also a pattern we have seen more broadly in humanitarian contexts, including in Syria. Organisations come in, install a system, and leave. When something goes wrong the system sits idle, sometimes never to be fixed. It is a large part of why we stay engaged long after the panels are up.
It is also why the hardware matters as much as the monitoring. We build our systems around high-quality batteries with a high number of discharge cycles. The more cycles a battery can handle, the longer and more reliably it runs. Remote monitoring and robust equipment are two halves of the same approach: a system that can operate autonomously, and be brought back online quickly when it cannot.
What the system makes possible
For a woman who has waited months, sometimes years, to reach a facility that can repair the injury that destroyed her social life and her sense of self, what matters most cannot be measured. But the scale of what reliable electricity unlocks is still worth stating:
Over the next ten years, this installation is estimated to save the clinic €71,945 compared to continued diesel dependency and avoid 258 tonnes of CO₂ emissions. The equivalent in cost terms, of around 1200 additional treatments.
Surgeries are already happening. The operating theatre at the Women's Village is now running on clean, stable solar power, consistently covering 93.7% of the facility's electricity needs.
A message from the ground:
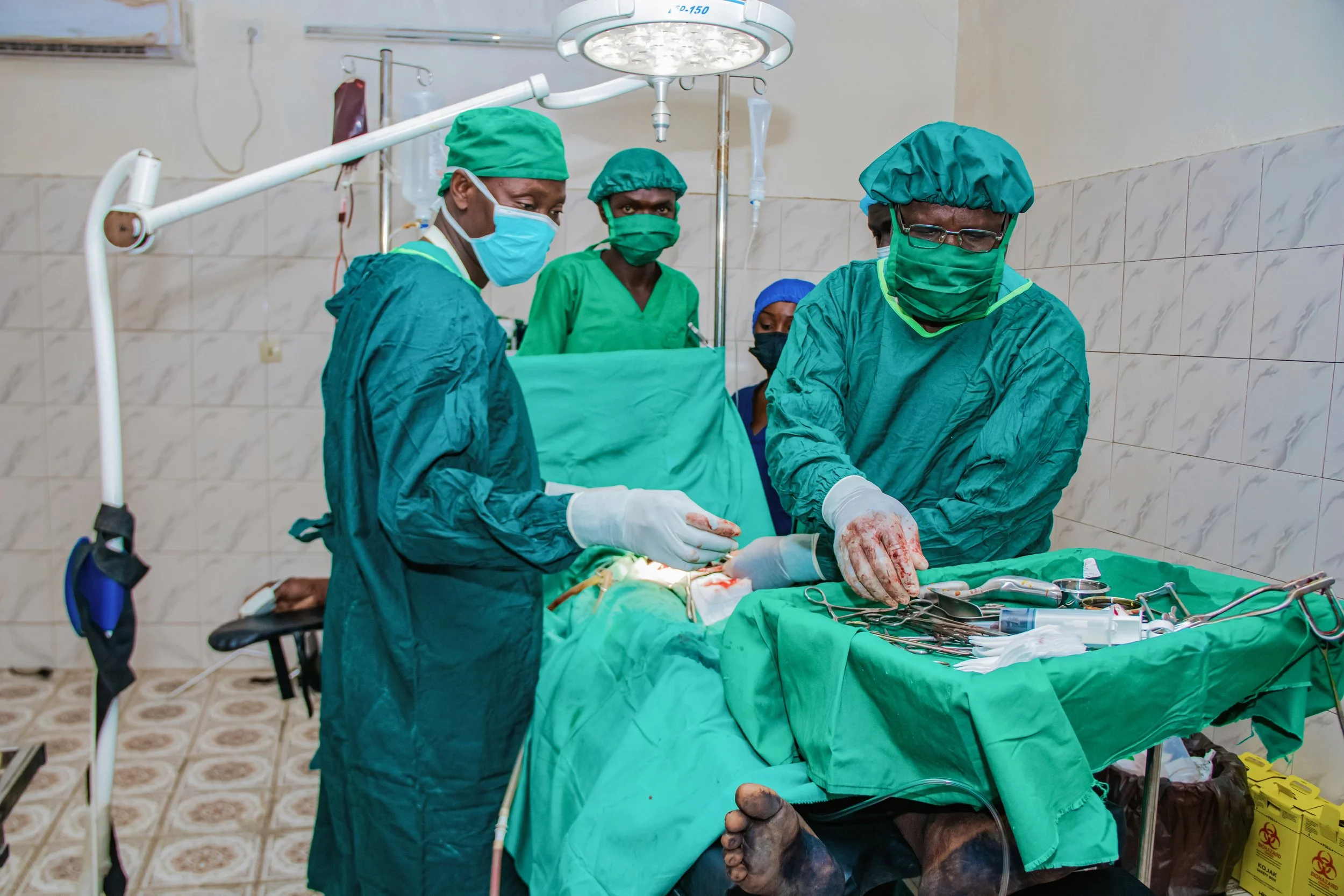
Routine operations continue at the Women's Village. Professor Dr. Valentin Vadandi and his team operated on a fistula survivor on Monday, 2 February 2026. Another survivor was treated on Tuesday 3 February. Post-operative monitoring of both patients revealed no complications. Two further survivors were scheduled to be treated on Wednesday, 4 February 2026.
Professor Dr. Valentin Vadandi and his team, working in the now solar powered operating theatre ©Kevin Doumdedje/ WHI
“The collaboration with Aidpioneers was always dynamic. Our respective organisations complemented each other quite nicely in this difficult task to ship and install the PV system in a very challenging environment.
I in particular appreciated the availability of Girmay Behre (Aid Pioneers’ Head of Solar Engineering) to assist our partner on the ground remotely even when there were language barriers.”
A model to replicate
The Women's Village project demonstrates what becomes possible when the right partners work together across the full chain: from diagnosis of need, through system design and delivery, to long-term support. Women’s Hope brought deep knowledge of the local context and a decade of trusted relationships on the ground. We brought technical expertise, logistics capability, and a team to stay engaged after installation.The system itself was designed to be fully autonomous, running without grid access through a hybrid inverter and high-quality batteries that supply power through the night, and operating independently of internet connectivity. Remote monitoring depends on it, but the system does not. It runs whether or not anyone is watching.
There are hundreds of facilities like the Women's Village across Sub-Saharan Africa. Facilities where dedicated healthcare workers are doing life-saving work under conditions that would be unacceptable anywhere with reliable power. Over 60% of Sub-Saharan African health facilities lack dependable electricity. For facilities beyond the reach of any national grid, solar is the only viable path to consistent, affordable power.
If you are an organisation, foundation or company looking to support health infrastructure in underserved regions, we would welcome a conversation about what is possible.
Patient consultation in a health post in the region. ©Salomon Djekorgee Dainyoo/ Women’s Hope / Fairpicture
Women’s Hope’s newly built hospitalization room at the Village des Femmes is also powered by the PV system.
The Aid Pioneers’ team during pre-shipment inspection in Chemnitz, Germany.
Unloading of the solar equipment at the Women's Village in Abéché.
The local installation team, Sahel BTP, during the installment of the system that spans two roofs.
The installed FOXess inverter.
Eastern Chad experiences Harmattan, a dry seasonal wind that carries lots of sand and dust, which means that panel cleaning is a routine part of operating the solar system. One of the realities of installing PV systems in the Sahel region.
Patient consultation in the region © Salomon Djekorgee Dainyoo/ Women’s Hope / Fairpicture.